Last week, the Medicare Rights Center explained how the House majority’s budget plan for 2019 would fundamentally restructure Medicare and Medicaid, slashing more than $2.1 trillion from the programs over 10 years. Though this approach is not unexpected—as lawmakers promised to use deficits created by last year’s tax bill as an excuse to pursue such cuts—it is extremely troubling.
Read More
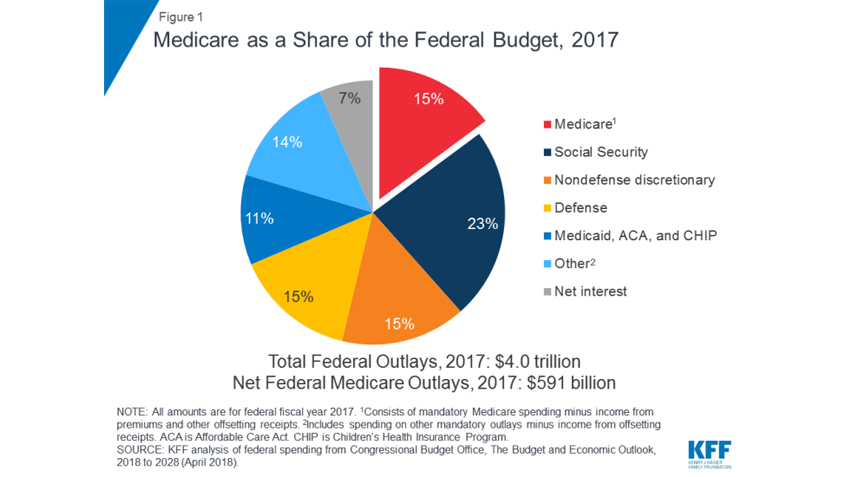
This week, the Kaiser Family Foundation released a new issue brief on Medicare spending. The brief analyzes the most recent historical and projected Medicare spending data published in the 2018 annual report of the Boards of Medicare Trustees and the 2018 Medicare baseline and projections from the Congressional Budget Office (CBO).
In 2017, Medicare spending accounted for 15% of the federal budget, and for 20% of total national health spending in 2016. It also accounted for 29% of spending on retail sales of prescription drugs, 25% of spending on hospital care, and 23% of spending on physician services.
Read More
This week, House Republicans unveiled a 2019 budget proposal that would balance the federal budget in nine years—largely by significantly cutting and fundamentally restructuring Medicare and Medicaid. This approach is not unexpected. Lawmakers were clear that after passing a costly tax bill that drives up deficits, they would use these higher deficits to justify cuts to programs like Medicare. In the House budget resolution, they are keeping that promise: the budget would end Medicare and Medicaid as we know them.
Read More
This week, the Health Policy Consensus Group—a consortium of think tanks and former and current lawmakers—put forward a new plan to repeal the Affordable Care Act (ACA) that would end Medicaid expansion and eliminate the ACA’s robust consumer protections for individuals with preexisting conditions, adults over 50, and women. If this sounds familiar, it should. Last year saw several plans to end the ACA’s Medicaid funding and consumer protections, often couched in language promising states more “flexibility.” These proposals would have caused millions of Americans to lose access to critical services, pay more for care, or even lose health coverage entirely.
Read More
Last week, the Department of Justice (DOJ) asked a federal court in Texas to end the Affordable Care Act’s (ACA) protections for people with pre-existing conditions. The underlying legal challenge was filed earlier this year by 20 state attorneys general, who argue that without the individual mandate—which was eliminated in December’s Tax Cuts and Jobs Act—the entire is ACA unconstitutional. In an unexpected move, the DOJ declined to defend the ACA in this case, and instead asked the court to invalidate only the law’s provisions that prevent insurers from denying coverage or charging higher rates based on health status.
Read More
In its annual report to Congress, the Board of Trustees for Medicare said the program’s hospital insurance trust fund (Part A) could lack funds to pay full benefits by 2026—three years earlier than projected in last year’s report. Despite this finding, the Medicare program itself remains strong and sustainable. The trustees report identifies several factors that impact the balance of program funds.
Read More
A draft handbook on Medicare enrollment has drawn criticism from senior’s advocates – and rightly so. The Centers for Medicare and Medicaid Services (CMS) released the draft for review in advance of mailing a final version to 43 million households this September. What bothers advocates is the handbook’s apparent bias toward private Medicare Advantage plans over traditional Medicare – using inaccurate and misleading information.
The Center for Medicare Advocacy, Justice in Aging, and the Medicare Rights Center have sent a letter to CMS Administrator Seema Verma, calling out “serious inaccuracies” in the draft handbook, entitled Medicare & You.
Read More