Today, the Medicare Rights Center released a report detailing the role consumer advocates and advocacy organizations can play in the implementation of health care reform efforts—known as health system transformation—designed to change how care is paid for and delivered to achieve improved quality and increased value of health care services in New York.
Read More
This week, Medicare Rights Center submitted comments on ways to eliminate red tape and bureaucracy in the Medicare program that affect how people with Medicare can access their care and benefits. These comments were generated in response to the “Medicare Red Tape Relief Project,” a request from Representative Pat Tiberi, the Chairman of the U.S. House Ways and Means Subcommittee on Health, for ideas to improve legislation or regulations to help “deliver relief from the regulations and mandates that impede innovation, drive up costs, and ultimately stand in the way of delivering better care for Medicare beneficiaries.”
Read More
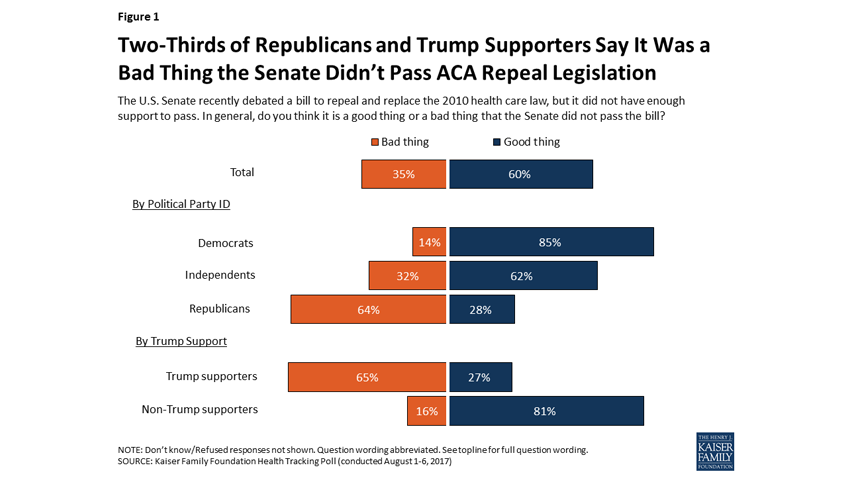
In the aftermath of the Senate’s failure to pass major health care legislation and repeal the Affordable Care Act (ACA), the Kaiser Family Foundation released findings from a poll to understand what Americans think of the ACA, the attempts to repeal it so far, and next steps.
Read More
This week, the Congressional Budget Office (CBO) released an analysis that found that ending payments to insurance companies to assist low-income Marketplace enrollees with health insurance costs would increase the deficit by $194 billion over 10 years. Under the Affordable Care Act (ACA), the federal government reimburses insurance companies for discounts on copays and deductibles the law requires insurers to give to low-income individuals.
Read More
The Centers for Medicare & Medicaid Services (CMS) recently announced that the average basic premium for a Part D prescription drug plan is estimated to be $33.50 per month in 2018. This projected average premium is a slight decrease from the average monthly premium in 2017 ($34.70) and represents the continued relative stability of Part D premiums. It is important to note that while the average, basic premium is lower in 2018, beneficiary premiums will vary—some increasing and some decreasing next year.
Read More
This week, a report for the Medicaid and CHIP Payment and Access Commission (MACPAC) examines the enrollment of likely eligible Medicare beneficiaries in Medicaid programs that assist with Medicare Part B premiums and cost-sharing, known as the Medicaid Savings Programs (MSPs). Using the most recently available data (2009 and 2010), the analysis shows that participation in the MSPs remains low.
Read More
Dear Marci,
Last year I received an Annual Notice of Change from my Medicare Advantage Plan. Will I get one this year? What should I do with it?
– Emmanuel (Springfield, MO)
Read More
Last week, Medicare celebrated 52 years since it was signed into law. In those 52 years, Medicare has provided guaranteed health benefits to millions of older adults and people with disabilities. Today, 57 million Americans and their families rely on Medicare for basic health and economic security and the program remains on solid footing.
Read More
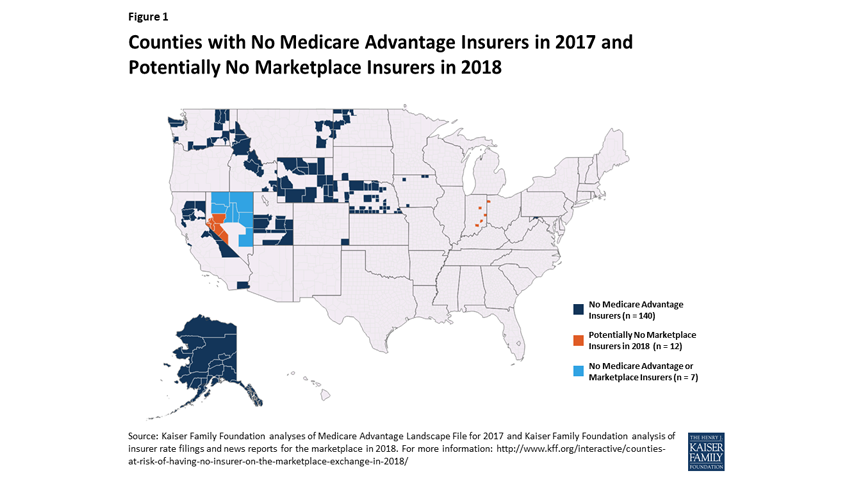
This week, the Kaiser Family Foundation (KFF) released a new issue brief examining a recent hot topic—areas with few or no insurers participating in Affordable Care Act (ACA) marketplaces. KFF compared these areas to places where there are very few or no Medicare Advantage (MA) plans offered this year to people with Medicare.
Nationwide, there are currently 19 counties—in Nevada, Indiana, and Ohio—that will have no ACA marketplace plans for sale in 2018. This number has been shrinking as insurers fill some of the gaps, so it is possible each of these counties will have coverage in 2018.
Read More