The Medicare Rights Center (Medicare Rights) responded to a request for information (RFI) from the Centers for Medicare & Medicaid Services (CMS) asking about inappropriate steering practices encouraging people into coverage that is not right for them. CMS raises concerns about whether providers, plans, or others who stand to gain from an individual’s enrollment decisions may improperly influence people who may be eligible for Medicare or Medicaid to decline public health insurance and retain private market coverage or convince people to give up private market coverage in favor of Medicare or Medicaid.
Read More
This week, 75 national organizations representing older adults, people with disabilities, insurers, health care providers, unions, and purchasers sent a letter to House and Senate Committee leaders highlighting recommendations regarding projected increases in Medicare Part B premiums and the Part B deductible in 2017.
Read More
A new bill, the Fair Drug Pricing Act, was introduced in both the Senate and the House this month promising to bring greater transparency to increases in drug prices.
Read More
In 1972, Medicare benefits were extended to cover the high cost of medical care for most individuals suffering from permanent kidney failure also known as end-stage renal disease (ESRD). People whose kidneys have failed need dialysis or a kidney transplant to live. To this day, kidney failure is one of only two medical conditions that gives people the option to enroll in Medicare without a two-year waiting period, regardless of age. Because Medicare for people with ESRD was established separately and later, there are some specific rules around eligibility and coverage of Medicare for dialysis and transplant patients.
Read More
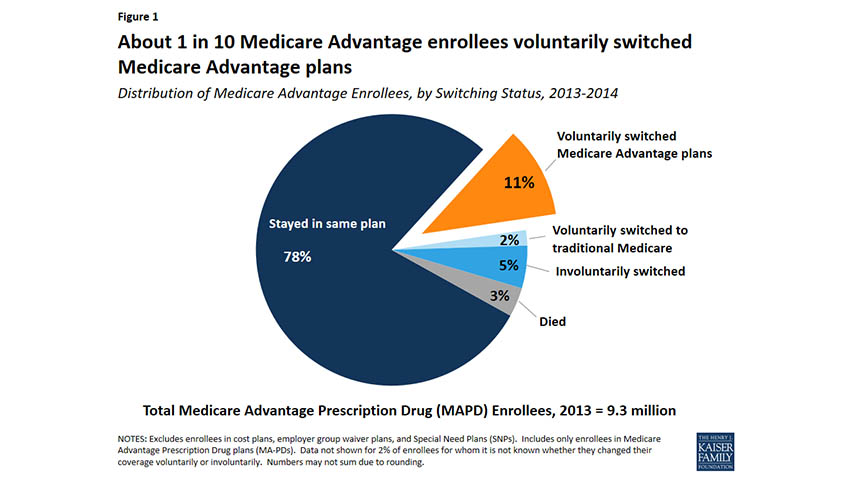
A new Kaiser Family Foundation (KFF) issue brief analyzes when people with Medicare make changes to their Medicare Advantage and Part D coverage. The paper highlights beneficiaries enrolled in Medicare Advantage plans with prescription drug coverage (MA-PDs) who change plans when given the opportunity.
Read More
Congress took steps this week to improve Medicare coverage and enrollment rules by introducing the “The Medicare Affordability and Enrollment Act of 2016.” If passed, the bill would create an out-of-pocket spending cap, reform the Medicare enrollment process by reducing penalties and gaps in coverage, and increase support for lower-income beneficiaries.
Read More
Dear Marci,
What changes can I make during Fall Open Enrollment?
– Herman (Chattanooga, TN)
Read More
As Medicare Fall Open Enrollment approaches, the time of year from October 15 to December 7 when people with Medicare can make changes to their coverage, the Medicare Rights Center submitted feedback and suggestions about a critical tool in making these decisions—the Medicare.gov Plan Finder.
Read More
Last week, the Medicare Rights Center submitted comments in response to proposals from the Centers for Medicare & Medicaid Services (CMS) to update and change aspects of the Physician Fee Schedule. This annual, proposed rule includes specific information about the payment rate for select services as well as broad policy initiatives and changes.
Read More
This week, Medicare Rights Center, along with a coalition of 20 organizations sent a letter expressing support for the mission and goals of the Centers for Medicare & Medicaid Innovation (CMMI), including the proposed Part B Drug Payment Model. CMMI is the part of the Centers for Medicare & Medicaid Services (CMS) tasked with developing and evaluating ways to make the Medicare program more value-driven, more efficient, and more effective at delivering and paying for needed care.
Read More