Among many measures in the Comprehensive Addiction and Recovery Act (CARA) of 2016, signed into law last week by President Obama, was a Part D “lock-in” program intended to prevent people with Medicare from misusing certain prescription drugs. The Medicare Rights Center played a pivotal role in shaping the program’s consumer safeguards along with its national partners.
Read More
This week, Joe Baker, president of the Medicare Rights Center, joined the honorable Sylvia Mathews Burwell, Secretary of the U.S. Department of Health and Human Services (HHS), for a roundtable discussion on how bundled payments can further ongoing efforts to transition Medicare from a volume-based payment system to one that reimburses for care coordination, quality, and innovation. Bundled payments are a reimbursement mechanism for the treatment of patients with specific conditions.
Read More
The Beneficiary Enrollment Notification and Eligibility Simplification (BENES) Act is bipartisan legislation to modernize the Part B enrollment process recently introduced in the House of Representatives and the Senate. Developed by the Medicare Rights Center and championed by Congressmen Raul Ruiz (D-CA) and Patrick Meehan (R-PA) as well as Senators Bob Casey (D-PA) and Chuck Schumer (D-NY), the bill aims to prevent costly Part B enrollment mistakes.
Read More
A recent issue brief from the Kaiser Family Foundation (KFF) answers important questions about a controversial Medicare savings proposal called premium support. KFF defines premium support as “a general term used to describe an approach to reform Medicare that aims to reduce the growth in Medicare spending by increasing competition among health plans and providing a stronger incentive for beneficiaries to be cost-conscious in their plan selection.”
Read More
The Medicare Rights Center is proud to offer a limited-time screening of You See Me, a heartfelt documentary from filmmaker Linda Brown.
The film is available through Medicare Interactive, the Medicare Rights Center’s online resource, from July 13 to July 27.
Read More
When President Obama took office in January 2009, one out of seven Americans had no health insurance. The Affordable Care Act (ACA) increased the number of insured by improving the accessibility, affordability, and quality of health care. This week, the President published a comprehensive article in the Journal of the American Medical Association (JAMA) outlining the positive results and improvements brought about by the ACA. Despite the innumerable developments brought to health care through the ACA, the President does not dismiss the fact that more is needed to carry forward the law’s promise.
Read More
A new report released by the Kaiser Family Foundation (KFF) highlights the demographics of people with Medicare who died in 2014 and the cost of care at the end of their life. The KFF findings on Medicare spending focus on people in traditional Medicare, since comparable data is unavailable for people enrolled in a Medicare Advantage plan. Still, the report findings contribute to the ongoing conversation about end-of-life care, what services people access at the end of life, and how much Medicare spends for those services.
Read More
Dear Marci,
My doctor recommended that I get a manual wheelchair to get around my home. Does Medicare cover wheelchairs? If so, what do I need to do so that they will cover it?
– Gabrielle (Bardstown, KY)
Read More
The U.S. House Subcommittee on Labor, Health and Human Services, and Education approved a bill that would provide funding for the State Health Insurance Assistance Program (SHIP) at the current level of $52.1 million, a measure applauded by the Medicare Rights Center. This comes after the Senate Appropriations Committee recently proposed eliminating SHIP funding altogether.
Read More
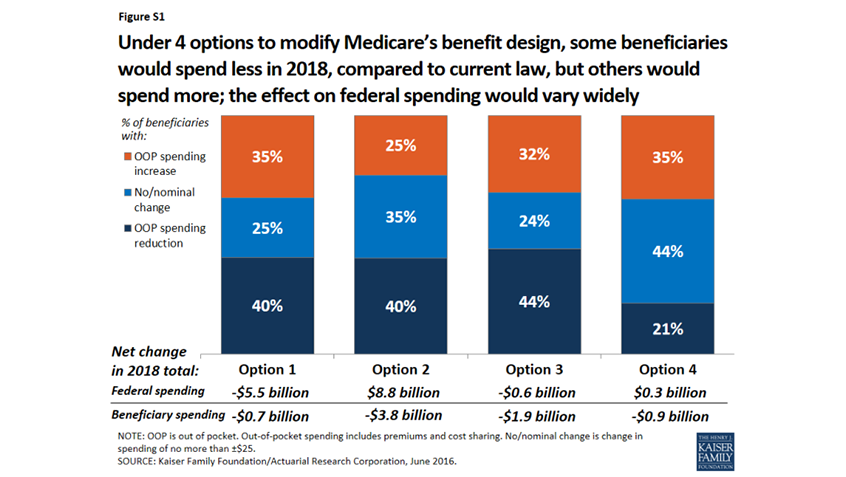
Last week, the Kaiser Family Foundation (KFF) released a report examining the anticipated effects of four options to modify Medicare’s benefit and cost-sharing design. The proposals include changes to the Medicare Part A and Part B deductible and cost-sharing amounts, as well as further restrictions to Medigap coverage. Each of the proposals are derived from policies proposed in recent years by the Congressional Budget Office (CBO), the Medicare Payment Advisory Commission (MedPAC), and other organizations
Read More